Update: July 15, 2022
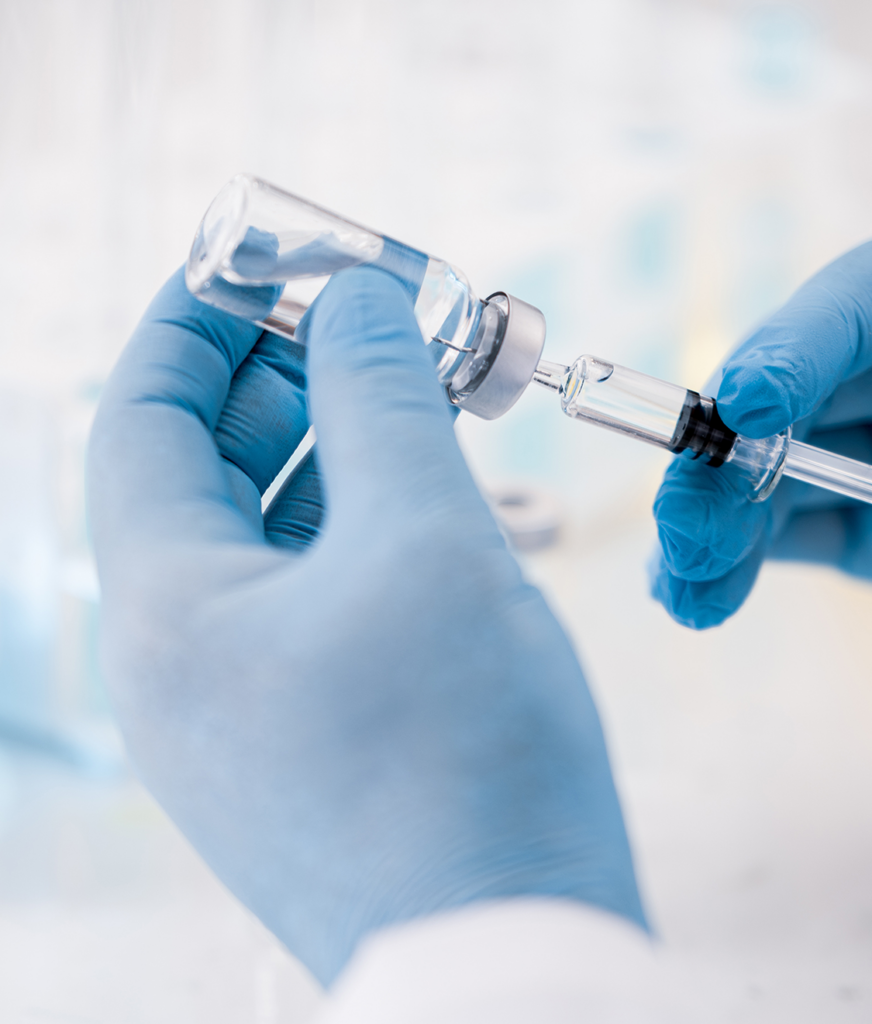
On Thursday, July 14, 2022 Health Canada approved the Moderna Spikevax Covid-19 vaccine for children aged six months to five years old. This makes approximately 1.7 million Canadian children eligible for vaccination. Health Canada has authorized a two-dose primary series of 25 micrograms each, with the second dose to be administered 4 weeks after the first dose. This is half the dose authorized for children six to eleven years old and one quarter of the dose authorized for people over twelve years of age.
Clinical trials were conducted during the Omicron surge and demonstrated that the vaccine is well-tolerated and had comparable efficacy to those in other age cohorts. While there is no specific information on children six months to five years old with type 1 diabetes, the vaccine is considered safe and effective. JDRF recommends speaking to your healthcare professionals if you have any questions or require more information.
***
On Friday, November 19, 2021, Health Canada approved the Pfizer/BioNTech vaccine for children 5-11 years old.
Parents now have the option to vaccinate their children against COVID-19.
Having type 1 diabetes (T1D) itself does not increase the risk of contracting the virus. As with any virus, however, there is the possibility for more severe health outcomes for kids with T1D, including hospitalization and increased potential for both hypo and hyperglycemic episodes.
As well, some children who contracted COVID-19 developed a rare but serious condition known as Multi Inflammatory Syndrome in Children (MIS-C). MIS-C results in the severe inflammation of some organs and tissues — like the heart, lungs, blood vessels, kidneys, digestive system, brain, skin, or eyes. Children, including those with T1D, can lower their risk of serious complications by receiving the COVID-19 vaccine.
The goal is always to try and prevent your child from getting ill in the first place. And with most kids back in school and activities, the possibility of encountering the coronavirus increases. The greater the number of people who are vaccinated, the lower the potential for community spread.
How are the children’s vaccines different?
The vaccine dose for children 5-11 is lower than the 12+ dosage – 10mcg versus 30mcg. Clinical trials with the Pfizer/BioNTech vaccine demonstrated significant antibody development at this dosage relative to the adult dose, showing a 90.7% efficacy against the virus.
The dosing schedule for Canadian children will be eight weeks between doses, as opposed to the three-week schedule currently being applied in the United States. NACI, the National Advisory Committee on Immunization, has recommended this dosing schedule under the assumption that it increases antibodies and may potentially lengthen the period between the second dose and antibodies waning.
It’s important to maintain the same measures (masking, handwashing, social distancing) between the two doses to try and prevent infection before the full series has been administered.
What if there are vaccine side effects?
Children may experience the same side effects as many adults: fatigue, muscle aches and chills, slight fever with headaches, and arm soreness.
Some adults with T1D found that the vaccine affected their blood sugar levels. Make sure to check your child’s blood sugar levels more frequently in the first few days after the vaccine to monitor for any potentials highs or lows that can be quickly managed.
When will vaccines be available for kids under five?
In September 2021, Pfizer CEO Albert Bourla announced that data on the COVID-19 vaccine for children between two and four years old should be available by the end of the year.
They are also currently running trials for infants six months to toddler (two-years-old), but there has been no announced timeline on when data from these trials will be made publicly available.
Until such time as full approval comes for all age groups, even after vaccination, it’s important to continue to maintain the same public health measures as before, masking in indoor spaces, good hygiene and handwashing, and limited interactions with crowds.
As with all health decisions, reach out to your child’s healthcare team to come to the decision that is best for your family.
Additional resources:
Canadian Pediatric Society: https://cps.ca/en/documents/position/covid-19-vaccine-for-children
Health Canada: https://www.canada.ca/en/public-health/services/vaccination-children/covid-19.html